Malaria, Plasmodium Falciparum, Plasmodium Malariae, Plasmodium Vivax, Plasmodium Ovale, Plasmodium Falciparum Infection, Plasmodium Malariae Infection, Plasmodium Vivax Infection, Plasmodium Ovale Infection, Ovale Malaria, Falciparum Malaria, Vivax Malaria, Quartan Malaria, Tertian Fever, Quartan Fever
- See Also
- Malaria Chemoprohylaxis
- Vector-Borne Infection
- Fever in the Returning Traveler
- Arbovirus
- Prevention of Vector-borne Infection
- Protozoa
- Epidemiology
-
Incidence
- Malaria is the most common life threatening disease for travelers
- Mosquito population is expected to as much as double with global warming (0.4 C) by 2020
- Europe and North America infections are typically due to travel
- European, North American traveler cases: 30,000/year
- U.S. Cases reported to CDC per year: 1500 to 2000 (out of 18 million U.S. travelers to Malaria endemic areas)
- Malaria was endemic to North America, but was eradicated in the mid-twentieth century
- Worldwide Infections: 300 million per year (up to 500 million/year)
- Children under age 5 years are disproportionately affected (esp. in sub-saharan africa)
- Chloroquine-resistant P. Falciparum Malaria kills 500,000 young children/year in Africa alone
- Worldwide Mortality: 1-3 Million deaths per year
- Malaria (esp. P. falciparum) is among the top three infectious causes of death in the world
- Other high mortality infectious causes include HIV Infection and Tuberculosis)
- Children under age 5 years are disproportionately affected (esp. in sub-saharan africa)
- Timing
- Majority of Malaria outbreaks occur between May and December
- Highest risk is during and after the rainy season
- River beds and stagnant pools of water are most common breading grounds
- Regions
- Endemic to tropical and subtropical world around the equator (106 countries as of 2010)
- Highest Risk
- Sub-Saharan Africa
- Papua New Guinea
- Solomon Islands
- Vanuatu
- Intermediate Risk
- Haiti
- Indian subcontinent
- Southeast Asia
- Low Risk
- Latin America
- Pathophysiology
- See Vector-Borne Infection
- Transmitted by bite of female anopheline (or anopheles) Mosquito
- Usually bites between dusk and dawn
- Injects malaria Protozoa from Salivary Glands
- Other modes of human transmission (e.g. Blood Transfusion, congenital transmission) are rare
- Species of Malaria
- Plasmodium Falciparum (most common and most life threatening)
- Fulminant Malaria associated with high Parasitemia and intravascular congestion
- Incubation Period: Typically 12-14 days (ranges from 7 to 30 days)
- Most severe of disease with multiorgan involvement (esp. brain, liver)
- Responsible for most Malaria deaths
- Irregular fever cycles (every 36 to 48 hours), or with Continuous Fever and symptoms
- Chloroquine resistance (except in central america)
- Sickle Cell Trait is partially protective against P. falciparum infection
- Sickle Cell Trait impedes Malaria RBC infection and survival within RBCs
- Plasmodium Vivax
- Incubation Period: Months to years
- Fever recurs every 3 days (Tertian Fever at 48 hour intervals) as with P. ovale
- May cause latent phase (hypnozoites), dormant within the liver for months to years
- P. vivax requires red cell surface Antigens Duffy A and B for binding
- Red cell Antigens Duffy A and B are absent in >60% of black patients (88-100% in West Africa)
- Absent Duffy A and B is protective against Plasmodium Vivax
- Plasmodium Ovale
- Incubation Period: Months to years
- Fever recurs every 3 days (Tertian Fever at 48 hour intervals) as with P. vivax
- May cause latent phase (hypnozoites), dormant within the liver for months to years
- Plasmodium Malariae (Quartan Malaria)
- Fever recurs every 4 days (Quartan Fever at 72 hour intervals)
- Plasmodium knowlesi
- Emerging pathogen in those exposed to macque monkeys
- Similar in appearance to p. Malariae
- As with Plasmodium Falciparum, may cause severe disease
- Plasmodium Falciparum (most common and most life threatening)
- Life cycle of Malaria
- Injected from Mosquito as sporozoite
- Sporozoites are thin, spindle shaped, motile forms of Malaria
- Sporozoites traverse the human bloodstream to the liver
- Sporozoites invade hepatocytes in human liver (Pre-erythrocytic cycle)
- Sporozoites undergo asexual division within hepatocytes
- Sporozoites may lie dormant in liver (hypnozoites)
- Occurs with Plasmodium Vivax and Plasmodium Ovale
- Symptoms recur when reactivates in months to years
- Merozoites develop from Sporozoites after weeks to months of development within hepatocytes (liver cells)
- Thin spindle shaped sporozoite transitions to a round form (trophozoite) within infected liver cells
- Trophozoite nucleus divides into thousands of nucleii, forming a Schizont within the liver cell
- Schizont nucleii each form cytoplasmic membranes creating small intracellular bodies (Merozoites)
- Engorged liver cells rupture, releasing merozoites into the bloodstream
- Merozoites invade erythrocytes and circulate freely
- P. Malariae may remain in Red Blood Cells without lysis, latent for months to years
- Typically results in Red Blood Cell lysis within 48-72 hours of erythrocyte invasion
- In severe cases (esp. P. falciparum), up to 30% of Red Blood Cells may be infected
- Merozoites form round trophozoites within the infected red cell
- Trophozoite appears as a ring with nuclear material clustered in one portion (diamond on a ring)
- Multinucleated schizont forms from cell division of the Trophozoite (similar to hepatic cell process)
- New merozoites form as each nucleus is surrounded by a cytoplasmic membrane
- Hemolysis (Red Blood Cell lysis) with schizont expansion
- Non-lysed, but infected RBCs also have increased adhesion to other RBCs and vascular endothelium
- Results in both vascular Occlusion as well as Hemorrhages
- May result in end organ injury (esp. P. falciparum), including brain, Kidney and lung
- Hemolysis is associated with fever spikes (and overall immune/inflammatory response)
- Fever spikes typically occur randomly, but may occur with RBC lysis in a pattern
- May cause Tertian Fever (recurring every third day as with P. ovale and vivax)
- May cause Quartan Fever (recurring every fourth day as with P. Malariae)
- Some circulating merozoites differentiate into male and female Gametocytes
- Gametocytes are the sexual form of plasmodium (sexually dividing within the Mosquito)
- Contrast with asexual division in the human liver
- Male and female Gametocytes circulate in the human blood stream
- Mosquito ingests both male and female gametocytes from infected host
- Oocysts develop within the Mosquito over a 10-21 day course into sporozoites
- Resulting sporozoites are motile, thin spindle-shaped Protozoa
- Sporozoites spread throughout the Mosquito, including the mosquito Salivary Glands
- Mosquito infects next human host with bite, transmitting motile sporozoites via its Saliva
- Gametocytes are the sexual form of plasmodium (sexually dividing within the Mosquito)
- Injected from Mosquito as sporozoite
- Precautions
- Fever in a returning traveler from Malaria endemic area is Malaria until proven otherwise
- Up to 50% of Malaria cases are misdiagnosed on the first visit
- Initial presentations are often mild and non-specific (fever, chills, malaise, myalgia, Headache)
- Malaria (esp. P falciparum) requires emergent evaluation
- Clinical decompensation or death may occur within 24 to 36 hours in a Malaria naive patient
- Symptoms
- Timing
- Presentation within the first month of return from travel to endemic region
- Plasmodium Falciparum Incubation Period is typically 12 to 14 days (range 7 to 30 days)
- See Fever in the Returning Traveler for timing of other illnesses in the differential
- Delayed presentation beyond 2 months may occur with the use of chemoprophylaxis
- Plasmodiun ovale and Plasmodium Vivax may have delayed presentations, months later
- Presentation within the first month of return from travel to endemic region
- Initial prodrome
- Headache
- Malaise
- Next
- Fever (>50% of patients)
- Shaking chills
- Drenching Night Sweats
- Next
- Drowsiness
- Lethargy
- Fatigue
- Other symptoms
- Myalgias
- More severe in Dengue Fever
- Muscle tenderness
- More severe in Leptospirosis and Typhus
- Arthralgias
- Back pain
- Gastrointestinal Symptoms (may be isolated presentation in children)
- Myalgias
- Signs
- Episodic fever for 1-8 hours
- May be persistent in P. falciparum
-
Fever recurs
- Plasmodium Vivax: 48 hour intervals (Tertian Fever)
- Plasmodium Malariae: 72 hour intervals (Quartan Fever)
- Plasmodium Falciparum: Variable
- Gastrointestinal findings (in <35-40% of cases)
- Increased splenic and hepatic activity results from Hemolysis
- Tender Splenomegaly (risk of Splenic Rupture)
- Hepatomegaly
- Severe Falciparum Malaria
- Hypotension and shock
- Multisystem failure
- Pulmonary Edema
- Acute Respiratory Distress Syndrome
- Renal Failure (1% of cases)
- Jaundice and liver failure (associated with poor prognosis)
- Cerebral Malaria
- Mortality approaches 15-20% in young children (<esp. age <5 years) even with treatment
- Altered Mental Status to unresponsive
- Seizures
- Meningism (uncommon but carries 23% mortality)
- Differential Diagnosis
- See Fever in the Returning Traveler
- See Vector-Borne Infection
- Arboviruses are also Vector-Borne Infections (Aedes aegypti Mosquito-Borne Disease is common vector)
- Rash is uncommon in Malaria (aside from Petechiae in severe Falciparum Malaria with DIC) and suggests other diagnosis
- Other Bacterial Infections
- Other Viral Infections
- Other Parasitic Infections
- Labs
-
Blood Glucose
- Hypoglycemia may occur (esp. children)
-
Complete Blood Count (CBC) with differential
- Especially consider Malaria with Leukopenia and Left Shift, Thrombocytopenia
- Hemoglobin or Hematocrit consistent with Anemia (29%)
- Leukopenia with White Blood Cell Count <5000/mm3 (26%)
- Thrombocytopenia (45%)
- Bandemia (85%)
-
Urinalysis
- Urobilinogen positive
- Hemoglobinuria (rare, may occur with Plasmodium Falciparum)
-
Cerebrospinal Fluid Examination
- Indicated in Altered Mental Status and fever
- Exclude Meningitis and Encephalitis (esp. if Malaria diagnosis is unclear)
- Malaria CSF is typically normal (aside from mild CSF Pleocytosis, mild increased CSF Protein)
- Diagnosis
-
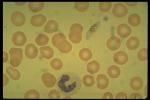
Peripheral Blood Smear
- Gold standard for diagnosis
-
Peripheral Smear is performed under oil-immersion, 1000x magnification
- Infected Red Blood Cells demonstrate intracellular trophozoites and schizonts
- Gametocytes may also be visualized in the peripheral blood external to RBCs
- Stains
- Giemsa stain (reference standard stain for Malaria evaluation with thick and thin smears)
- Thin blood smear (first-line Malaria evaluation)
- Giemsa stain of blood fixed with Alcohol to prevent Red Blood Cell lysis
- Thin stain can identify Malaria species and quantify Parasitemia
- High Test Sensitivity
- Thick blood smear (perform if thin blood smear negative)
- Giemsa stain of blood allowed to dry on slide (allowing cell lysis)
- Thick stain evaluates for malaria Parasites in general
- Thin blood smear (first-line Malaria evaluation)
- Wright stain (standard stain for most Complete Blood Count associated manual differentials)
- Test Sensitivity approaches that of Giemsa stain
- Giemsa stain (reference standard stain for Malaria evaluation with thick and thin smears)
- Protocol
- Stat blood smear with direct communication with reading pathologist (alert for Malaria concern)
- Examine new smear every 12-24 hours for 2-3 days (low Parasitemia may require additional smears)
- Sample is best obtained when patient is febrile
- Image
- Rapid blood dipstick testing (when smear not available)
- Tests
- Binax-NOW (only detect P. falciparum and P. vivax; only FDA approved test in U.S.)
- HRP-2 detection (only detects P. falciparum)
- LDH detection (detects all 4 Malaria types)
- Benefits
- Good Test Sensitivity and Negative Predictive Value, yet easy to perform and does not require lab facility
- Results available within 5 to 20 minutes
- Precautions
- All rapid tests should be followed by blood smears
- Positive tests do not quantitate Parasitemia
- Negative rapid tests should be confirmed with blood smears
- Decreased Test Sensitivity with low levels of Parasitemia
- Examples: Patients who took chemoprophylaxis, or prior exposure
- All rapid tests should be followed by blood smears
- Tests
- Malaria PCR
- Detects low levels of parsites in blood (<5 Parasites/ul)
- Distinguishes between plasmodium species
- May be used to monitor response to treatment at 5-8 days (however False Positives may occur)
- Management
- Falciparum or Knowlesi Malaria or Severe Case and Unknown Species
- See CDC emergency contact information as below for Malaria management guidance
- Precautions
- Substandard and counterfeit antimalarial use is widespread in resource limited and low income countries
- G6PD Deficiency
- Avoid Chloroquine, Primaquine, Quinine (due to Hemolysis risk)
- Anti-Malarials Considered safe in Pregnancy
- Chloroquine
- Hydroxychloroquine
- Quinine or Quinidine
- Clindamycin
- Mefloquin
- Sulfadoxine Pyrimethamine (second and third trimesters only)
- Artemisinin Combination Therapy (ACT) safe in second and third trimester
- Artemether/Lumefantrine (Coartem) may be used in first trimester if no other reasonable option
- Hospital Admission Criteria
- Admit P. Falciparum Malaria and P. Knowlesi cases to hospital (high mortality in first 48 hours)
- Also admit all undiferentiated cases where species of Malaria cannot be discerned
- High Risk Cohorts
- Immunocompromised
- Malaria naive patients (no prior Malaria infections)
- Children
- Pregnancy
- Severe case criteria (any of the following)
- Glasgow Coma Scale (GCS) <11 or Coma
- Seizures
- Severe Anemia (Hemoglobin <7 g/dl in adults, <5 g/dl in children age <12 years)
- Acute Kidney Injury
- Hypoglycemia
- Acute Respiratory Distress Syndrome
- Shock
- Disseminated Intravascular Coagulation
- Acidosis
- Liver Dysfunction
- Parasite Density >5%
- Admit P. Falciparum Malaria and P. Knowlesi cases to hospital (high mortality in first 48 hours)
-
Artemisinin Combination Therapy (ACT) Antiparasitic Agents (2 agents)
- Regimens based on severity (see above for severe case criteria)
- General Protocol
- Agent 1: Artemisinin (or dihydroartemisinin, Artemether, or Artesunate) - first-line agent
- See Artesunate (preferred in U.S.)
- Artemisinin is contraindicated in first trimester of pregnancy
- Use oral formulation in non-severe cases, and intravenous formulation in severe cases
- Agent 2: Lumefantrine (see below), Chloroquine, Sulfadoxine-Pyrimethamine (Fansidar) or Mefloquine
- Treat for 3 days (6 days if travel to areas with high Malaria resistance)
- Agent 1: Artemisinin (or dihydroartemisinin, Artemether, or Artesunate) - first-line agent
- Non-Severe Cases: Artemether/Lumefantrine (Coartem)
- Each tablet contains 20 mg Artemether (an Artemisinin) and 120 mg Lumefantrine
- Tablets may be crushed and mixed with 10 ml water if unable to swallow tablets (e.g. children)
- Tablets are best absorbed with high fat foods
- Repeat dose if Vomiting occurs within 2 hours of dose
- Each dose based on weight
- Children 5 kg to 15 kg: 1 tablet per dose
- Children 15 kg to 25 kg: 2 tablets per dose
- Children 25 kg to 35 kg: 3 tablets per dose
- Children >35 kg and Adults: 4 tablets per dose
- Dosing (3 day course, with doses per weight as above)
- Give one dose every 8 hours for 2 doses on day 1, then one dose every 12 hours on days 2 and 3
- Each tablet contains 20 mg Artemether (an Artemisinin) and 120 mg Lumefantrine
- Severe Cases: Intravenous Artemisinin (Artesunate is preferred)
- Indicated in severe cases (see criteria above), including Parasite load >5%
- Start immediately at the time of diagnosis
- Artesunate 2.4 mg/kg at start, 12 and 24 hours, then daily until Parasitemia <1% (up to 7 days)
- Obtain blood smear Parasite stains for density every 12 hours
- Other agents when Artemisinin Combination Therapy (ACT) is unavailable
- Chloroquine sensitive regions
- Chloroquine
- Adults
- Load: 1000 mg salt (600 mg base) orally at start
- Maintenance: 500 mg salt (300 mg base) orally at 6 hours, 24 hours and 48 hours after initial dose
- Child
- Load: 16.7 mg/kg salt (10 mg/kg base) orally at start
- Maintenance: 8.3 mg/kg salt (5 mg/kg base) orally at 6 hours, 24 hours and 48 hours after initial dose
- Adults
- Hydroxychloroquine (Plaquenil)
- Adult: 800 mg salt (620 mg base) to start, then 400 mg salt (310 mg base) at 6, 24 and 48 hours after initial dose
- Child: 12.9 mg/kg salt (10 mg/kg base) to start, then 6.5 mg/kg salt (5 mg/kg mg base) at 6, 24 and 48 hours after initial dose
- Chloroquine
- Chloroquine resistant regions
- Atovaquone/Proguanil (Malarone)
- See Atovaquone for dosing
- Quinine-based protocols (2 agents)
- General
- Avoid in severe disease
- Use 7 day course if acquired in Southeast Asia
- Quinine 10 mg/kg up to 648 mg salt (8.3 mg/kg up to 542 mg base) three times daily orally for 3 to 7 days AND
- Second Agent
- Doxycycline 2.2 mg/kg up to 100 mg orally twice daily for 7 days (or Tetracycline) OR
- Clindamycin (if Tetracyclines contraindicated) 20 mg/kg orally for 3 to 7 days
- General
- Mefloquine (other options are preferred)
- Adult: 750 mg salt (684 mg base) for first dose, then second dose of 500 mg salt (456 mg base) in 6 to 12 hours
- Child: 15 mg/kg salt (13.7 mg/kg base) for first dose, then second dose of 10 mg/kg salt (9.1 mg/kg base) in 6 to 12 hours
- Atovaquone/Proguanil (Malarone)
- Chloroquine sensitive regions
- Plasmodium Malariae and Plasmodium knowlesi
- Artemisinin Combination Therapy (ACT) is recommended despite lack of Chloroquine resistance (see protocol below)
- Admit all Plasmodium knowlesi cases (high risk for severe disease)
- Following Initial Treatment: Plasmodium Ovale or Plasmodium Vivax (risk of relapsing infection)
- Risk of dormant Malaria (due to hypnozoites) and relapsing infection
- Follow initial course with following therapies to prevent relapsing infection
- Mothers infected with P. vivax or P. ovale during pregnancy
- Test infants for G6PD Deficiency after delivery
- Mothers should Breast feed and take either Primaquine (No G6PD Deficiency) or Chloroquine (G6PD deficient)
- No G6PD Deficiency
- Primaquine
- Adult: 52.6 mg salt (30 mg base) orally daily for 14 days after initial course
- Child: 0.8 mg/kg salt (0.5 mg/kg base up to 30 mg/day) orally daily for 14 days after initial course
- Decrease dose if Tinnitus or hyperexcitability occur
- Tafenoquine
- Adult (>age 16 years): 300 mg orally once after first or second day following Chloroquine course
- Contraindicated age <16 years or Psychotic Disorder
- Use only if Chloroquine or Hydroxychloroquine were used to treat initial infection
- Primaquine
- G6PD Deficiency
- Continue Chloroquine prophylaxis 500 mg salt (300 mg base) dosed weekly for one year OR
- Primaquine may be considered if G6PD is mild or intermediate
- Consult infectious disease
- Risk of dormant Malaria (due to hypnozoites) and relapsing infection
- Specific complication management
- Shock
- Intravenous hydration (including fluid boluses)
- Obtain Blood Cultures and add Third Generation Cephalosporin to regimen
- Cerebral Malaria (18% of cases)
- Seizures
- Supportive care including intubation may be needed
- Meningism (see above, uncommon but carries 23% mortality)
- Bleeding
- Coagulopathy reversal
- Blood Transfusion
- Shock
- Other non-specific management
- Intravenous Fluids
- Antipyretics
- Antiemetics
- Follow-up
- Evaluate for Hemolytic Anemia at 30 days after treatment of severe cases
- Prevention
- Malaria specific prevention
- Malaria Chemoprophylaxis is critical and not taken adequately in as many as 75% of U.S. travelers
- Malaria Vaccine
- WHO has recommended use for Malaria falciparum prevention in children
- Vaccination initiated in 2021 in Ghana, Malawi and Kenya (>1 million doses administered as of 2022)
- Alonso (2022) N Engl J Med 386(11): 1005-7 [PubMed]
- Prevent anopheles Mosquito Bites
- See Prevention of Vector-borne Infection
- Stay in air conditioned or well screened rooms
- Reduce nighttime outdoor activity (Dusk until dawn)
- Apply an effective Insect Repellent
- DEET 20 to 30% to skin every 3-4 hours or
- Picaridin 20% or
- p-Menthane-3,8-diol (PMD, Menthoglycol)
- Spray clothing and bed nets with Permethrin
- Wear long sleeve shirt and pants
- Use Insecticide aerosols at dusk in living areas
- Use a strong fan at bedside
- Use Mosquito bed netting even in hotel rooms
- Mosquito net pre-treated with Permethrin
- Reapply Permethrin every 6 months
- Complications
- Encephalopathy (Cerebral Malaria)
- Seizures and coma
- High mortality (esp. children)
- Hypoglycemia
- Acute Renal Failure
- Hepatic Dysfunction
- Pulmonary Edema
- Disseminated Intravascular Coagulation
- Hemolytic Anemia
- Shock
- Prognosis
- Plasmodium Falciparum Mortality: 4% (20% in severe cases)
- More severe cases in children and pregnant women
- Resources
- See Travel Resources
- CDC Malaria hotline (health care professionals)
- https://www.cdc.gov/parasites/contact.html
- Phone: 770-488-7788 (daytime, Monday to Friday, 9 am to 5 pm Eastern Standard Time)
- Phone: 855-856-4713 (daytime, toll free)
- Phone: 770-488-7100 (after hours, emergency operations center, ask to speak with DPDM expert)
- CDC Malaria Information
- Malaria Foundation International
- References
- Gladwin, Trattler and Mahan (2014) Clinical Microbiology, Medmaster, Fl, p. 343-6
- Anderson (2014) Crit Dec Emerg Med 28(7): 11-9
- Black, Martin, DeVos (2018) Crit Dec Emerg Med 32(8): 3-12
- Mason and Marsh in Herbert (2019) EM:Rap 19(5):12-3
- Nordurft-Froman and DeVos (2022) Crit Dec Emerg Med 36(4): 4-15
- Baird (1999) Med Clin North Am 83(4):923-44 [PubMed]
- Croft (2000) BMJ 321(7254):154-60 [PubMed]
- Feder (2013) Am Fam Physician 88(8): 524-30 [PubMed]
- Johnson (2012) Am Fam Physician 85(10): 973-7 [PubMed]
- Lo Re (2003) Am Fam Physician 68(3):509-16 [PubMed]
- Shahbodaghi (2022) Am Fam Physician 106(3): 270-8 [PubMed]