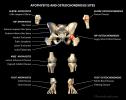
Apophyseal Injury, Apophysitis, Apophyseal Fracture, Traction Apophysitis
- See Also
- Definitions
- Apophysis
- Secondary ossification sites for tendon insertions
- Apophysitis
- Apophyseal inflammation prior to Growth Plate closure
- Epidemiology
- Apophysitis is seen most commonly in young athletes
- Pelvis is the most common site of Apophyseal Fracture
- Pathophysiology
- Causes
- Extremities
- Elbow
-
Knee
- Inferior Pole of Patella (Larsen-Johansson Disease)
- Tibial Tubercle Apophysitis (Osgood-Schlatter Disease)
-
Foot
- Calcaneal Aphophysitis (Sever's Disease)
- Fifth Metatarsal aphophysitis (Iselin's Disease)
- Causes
- Pelvis
- Anterior Superior Iliac Spine
- See Anterior Superior Iliac Spine Avulsion Fracture
- Sartorius tendon insertion
- Anterior Inferior Iliac Spine
- See Anterior Inferior Iliac Spine Avulsion Fracture
- Rectus Femoris tendon insertion
- Ischial tuberosity
- Hamstring tendon insertion
- Iliac Crest
- Transverse abdominis insertion
- External oblique insertion
- Internal oblique tendon insertion
-
Pubic Apophysitis
- Pubic Symphysis
- Gracilis tendon insertion
- Hip adductors insertion
- Signs
- Localized swelling and pain at given apophysis
- Provoked by contraction against resistance of the involved tendon insertion
- Imaging
-
XRay
- Differentiates Apophysitis from avulsion Fracture, Stress Fracture, Bone Tumor, Osteochondrosis
- Ulrasound
- Widened and fragmented apophysis
- Differential Diagnosis
- Traumatic Injury
- Stress Fracture
- Avulsion Fracture
- Bony Lesions (e.g. Cancer)
- Osteomyelitis
- Inflammatory Arthropathy (multiple joints involved)
- Management
- See specific Apophysitis causes
- Conservative therapy is effective in most cases
- Self-limited, resolving as flexibility improves and Growth Plates close
- Stretching
- Relative rest with cross-training to other activities
- Ice Therapy
- NSAIDs (judicious use)
- Orthopedic or sports medicine Consultation indications
- Pain persists after apophysis fusion
- Symptoms refractory to conservative management
- Red Flags (severe pain, Trauma, inability to bear weight, night pain, systemic symptoms, cancer history)
- Prevention
- Avoid over-training and overuse
- Keep pre-high school sports involvement broad without specialization
- Encourage cross training